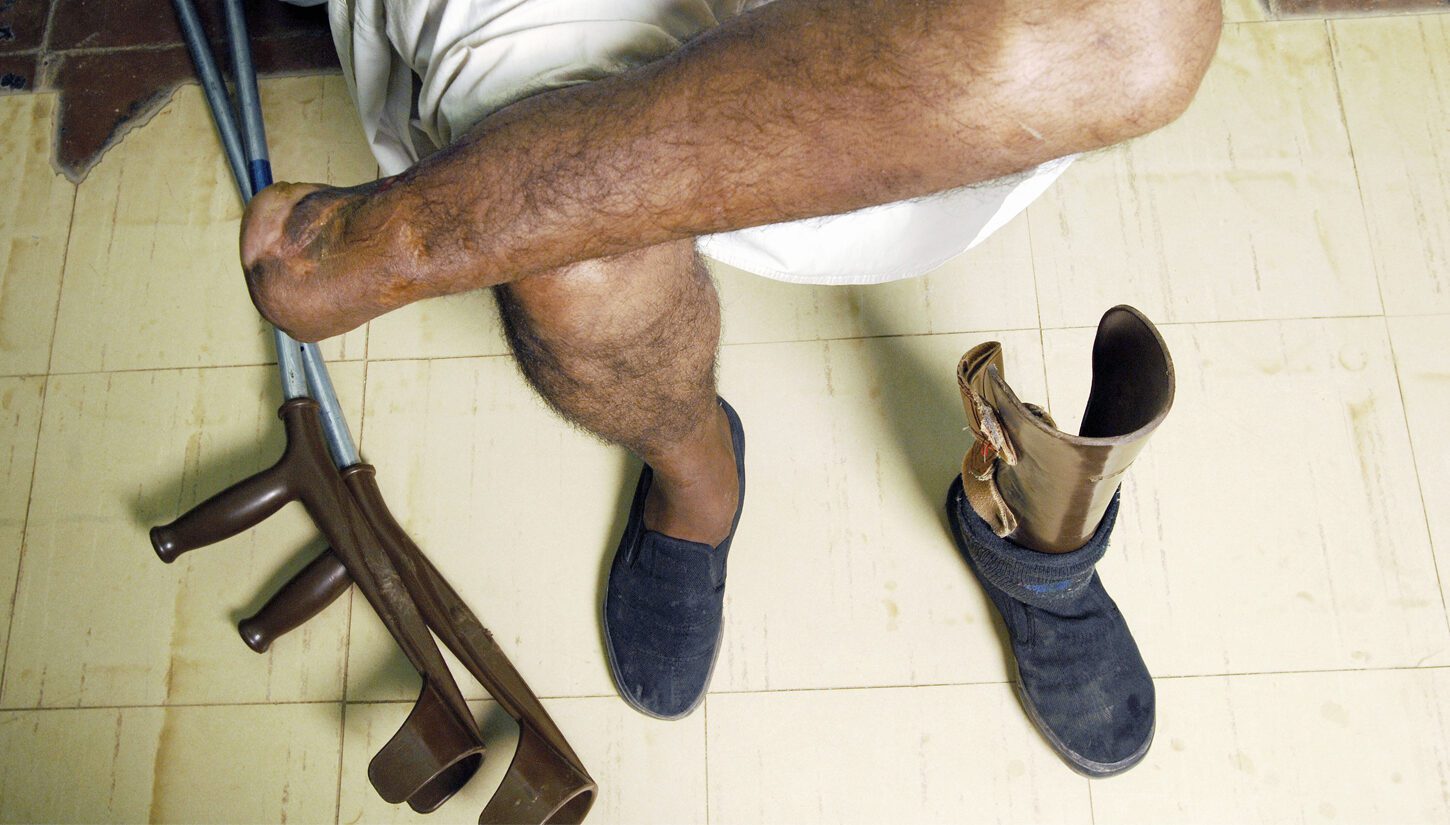
Mycetoma is an infectious disease endemic to tropical regions which can lead to severe deformities and, in some cases, to amputations. A quick diagnosis and the appropriate therapy can avoid a considerable amount of suffering. For this reason, scientific researcher Wendy van de Sande and her international team are working on the development of a user-friendly testing tool.
Mycetoma is a condition that occurs mainly in tropical and subtropical regions. ‘Many people walk barefoot there,’ Van de Sande explains. ‘If a person steps on a thorn, it is possible that the fungus or the bacteria which causes mycetoma could be transferred to the foot through the wound. The infected person wouldn’t even realise it, not even if the so-called grain, a tiny ball in which the fungus or bacteria reside, were to form in the tissue.’ Once infected, large tumour-like lesions begin to form on the feet. Moreover, the infection penetrates the bone. At this stage, the infection is relatively painless, but of course it increasingly starts to hinder the patient’s movement. In most cases, only then will people decide to visit a medical centre. ‘Often, patients must travel for several days in order to reach a specialised clinic for a diagnosis and treatment. Occasionally, treatment can provide a cure, but more often than not, the only solution is amputation. This tends to lead to exclusion from society and the loss of employment.’
In Africa, an estimated 6 in 1,000 people suffer from mycetoma. By starting therapy too late, 25 percent of them will require an amputation.
Fungal infection
An early diagnosis is essential. Van de Sande: ‘In the first instance, a doctor has to determine whether the infection is bacterial or fungal. In order to do that, we must isolate a specific part of the DNA.’ The treatment of a bacterial infection, even at a later stage, is easy; for 90 per cent of cases, the prescribed treatment will provide a cure. In contrast, the fungal infection is far more harmful. ‘We are currently working together with a specialist clinic in Sudan. They have visited 25 villages and they estimate that six out of every thousand people there are infected. Of these, at least a quarter will have to deal with an amputation.’
Therapy
In collaboration with other international partners such as the Centers for Disease Control in Atlanta, Newcastle University as well as clinics in Sudan and Senegal, Van de Sande is hoping to have developed a test tool within three years – one that will not only diagnose the type of infection, but one that will also provide the doctor on duty with information on the best way to treat the infection. ‘The test can be applied in locally-operated hospitals in Africa which have limited resources. It is comparable with the PCR test used to diagnose COVID-19. As soon as you have the DNA, the results and the necessary treatment will be known within half an hour. That is a feasible time frame when you travel with a medical team from village to village in rural areas.’
Clinical trials
If the testing tool proves to meet expectations, clinical trials can begin. ‘Then, we will roll out the test over a wide area in order to gather more data. If the data confirms the test’s reliability, then we will start looking for partners willing to develop the test commercially, in order to make it available to various medical centres in Africa, as well as South and Central America, for example. The ultimate goal would be to include the test tool in the WHO programme.’